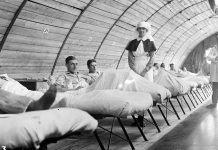
A major nurse-led trial to see whether aspirin could aid the healing of the often painful and disabling venous leg ulcers has found it made no impact.
Results of the randomised controlled trial, lead by nurse and University of Auckland Associate Professor Andrew Jull, have just been published in the British Medical Journal.
Nursing Review last year reported on the research project – one of New Zealand’s first ever nurse-led the randomised controlled trials (RCTs) – and Jull’s hope that low-dose aspirin might help prove a new treatment to aid the slow-healing wounds.
But the Aspirin4VLU trial – funded by the New Zealand Health Research Council and conducted by Jull and other researchers at Auckland’s National Institute for Health Innovation – found 150 mg aspirin a day, in addition to the proven treatment of compression bandaging, did not increase venous ulcer healing.
Seven out of every 10 people with leg ulcers who took aspirin healed within six months compared with eight out of every 10 people in the placebo group.
Jull said while he had hoped aspirin might help with healing, it was still good news. “It means people who have a venous leg ulcer and who have to take aspirin for other reasons still heal at a pretty good rate if they use compression.”
The trial had kicked off in March 2015 in district nursing services in five centres around the country: Auckland, South Auckland, Waikato, Christchurch and Dunedin. Each centre had a senior site investigator – a senior nurse who was a wound care specialist – and a part-time research nurse seconded from the district nursing team. Just over 250 participants were recruited to the trial.
Jull said the researchers would shortly be getting in touch with the participants to let them and their doctors know which drug they were taking. “We remain very grateful to those people who came forward to be part of the study – without them we would not have the evidence to help others.”
About 1 percent of the adult population will develop a venous leg ulcer during any one year. Compression therapy, either in the form of bandage systems or hosiery, is the main treatment. But in trials of venous leg ulcers about half the participants remain unhealed after three months of treatment.
Jull told Nursing Review last year that the research was prompted by the belief that aspirin might aid venous leg ulcer (VLU) healing because firstly VLUs result from chronic venous insufficiency (CVI), which is associated with platelet aggregation, and aspirin is known to inhibit platelet aggregation. Secondly, aspirin might also have an effect on the underlying inflammatory pathway associated with ulcers.
Aspirin4VLU is the world’s largest aspirin trial yet conducted for patients with venous ulcers and the only trial of low dose aspirin.