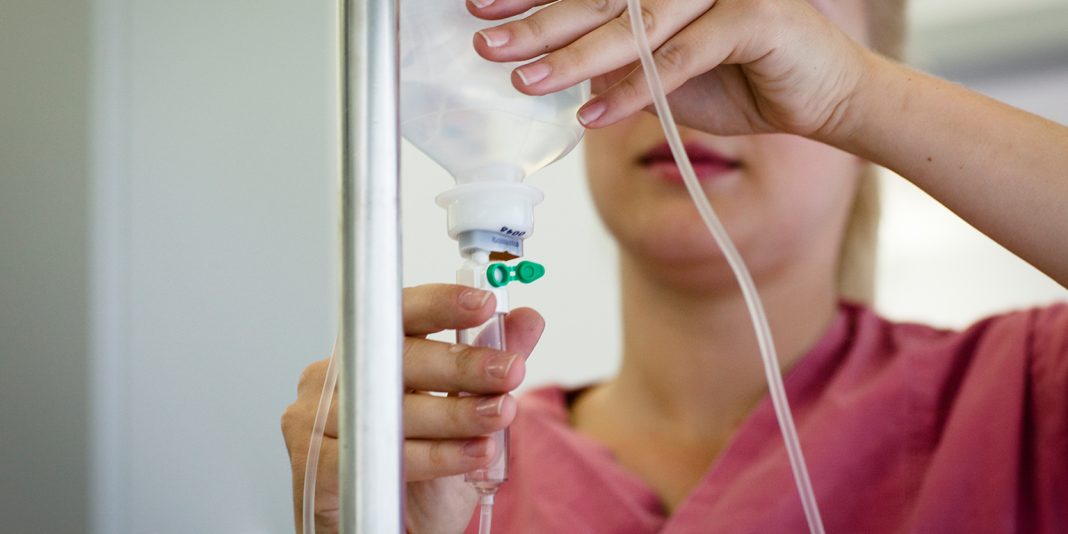
A newborn faced having plastic surgery on her arm after failures in IV nursing care and a registrar over-prescribed IV fluids, a Health and Disability Commissioner inquiry has found.
The Deputy Health and Disability Commissioner Rose Wall this week released a report finding Bay of Plenty District Health Board and two registered nurses in breach of the Code of Health and Disability Services Consumers’ Rights (the Code) for failings in the care provided in 2015 to the baby in its hospital.
The baby, just seven days old when admitted for jaundice, had to be transferred to the neonatal intensive care unit of another DHB where a plastic surgeon was consulted following blisters, swelling and an extravasation injury resulting from IV fluid and antibiotic treatment while in BoPDHB’s care.
Wall says in her report that amongst the failings (see full case study, findings and recommendations below) was that a junior paediatric registrar had prescribed IV fluids at a much higher rate than recommended by the DHB’s own policy and other national guidelines. Multiple staff reviewed the baby but did not pick up that her IV fluids were too high and also multiple staff failed to fill in the baby’s fluid balance chart in accordance with the policy requirements.
She found the afternoon shift nurse (RN B) in breach of the Code for not carrying out the hourly IV site monitoring and documentation required, not documenting an issue with the IV pump alarm or alerting the night shift nurse about the problem. Wall found the night shift nurse in breach for failing to review the baby’s IV site for two hours at the start of her shift and failing to document the phlebitis and infilitration scores.
Amongst the HDC recommendations (see below) was that the DHB use the incident as an anonymous case study for the induction of nursing and medical staff to the children’s ward and neonatal unit.
The DHB reported to the HDC that after its own investigation in 2015 it had carried out a number of actions, including asking all nurses to read and sign the DHB’s paediatric fluid balance protocol, education updates on IV luers, documentation and fluid balance charts for nurses, and the Children’s Ward now undertakes monthly audits of IV access.
RN B told the inquiry that on the shift in question her husband had rung and asked whether she could come home to look after a sick family member, but the ward was extremely busy so she decided to stay.
She acknowledged her documentation that shift was poor but said she had been checking the baby frequently as she knew “full well the higher rate of extravasation injury in neonates” and if there had been any obvious tissuing she would not have hesitated to remove the line. RN B formally apologised to the family for her part in the incident and said she and her colleagues had “learnt a valuable lesson about neonatal infiltration risks and the need for clear and concise documentation”.
RN C also apologised and said she had spent many hours reflecting on what happened. She said she had made changes to her practise in response, including redoing her IV certification, being prepared to delegate tasks if a shift is busy (as it was on the night in question) and being much more vigilant in checking the dosage of IV fluids and antibiotics, even if infusion has begun before she takes over a shift.
CASE SUMMARY
A seven-day-old baby was taken to the emergency department by her parents in the evening (Day 1) after paediatric advice was sought by their midwife because the baby was showing signs of jaundice.
The baby was triaged at 10pm and then reviewed at midnight when it was recorded she had had 11% weight loss since birth, jaundice, and reduced feeding. At around 2.40am the baby was admitted to the children’s ward (the special care baby unit was at full capacity) and was treated with phototherapy.
At nearly midday (now Day 2), the baby’s temperature spiked. The consultant paediatrician ordered investigations to try to determine the cause, and after the baby had several episodes of apnoea it was decided to commence intravenous (IV) fluids and antibiotics. A junior paediatric registrar (Dr D) prescribed the antibiotics and IV fluids. The registrar prescribed IV fluids at a rate of 180ml/kg/day, which was higher than the amount recommended by the DHB’s policy and other national guidelines.
On the morning of Day 3, the baby was reviewed and it was recorded that the septic screen was negative, but IV antibiotics and fluids would be continued, and that a fluid balance chart would be maintained.
RN B cared for the baby on the evening shift of Day 3. During the shift, the nurse administered the baby’s antibiotics then recommenced the IV fluids. At about 8.30pm the IV monitor began to flash, saying that there was a “downward occlusion”. RN B and a senior nurse investigated the line and the IV site but did not find any obvious issues. RN B did not clearly document the issues she had with the IV line during the shift, nor did she hand these over to the following shift.
Another registered nurse (RN C) took over the baby’s care at 11.15pm for the night shift but did not review the baby for nearly two hours. At around 2.30am, the baby was due for her next antibiotics. The nurse said that there were no signs of phlebitis or tissue infiltration when she commenced the first IV antibiotic. During the administration of the antibiotic, the baby’s mother noted a blister forming on the baby’s upper arm, and yelled for the nurse as the arm started swelling immediately. RN C stopped the antibiotic infusion and called for assistance. The baby was reviewed by a senior house officer and treated for an extravasation injury (caused by the IV antibiotic going into the tissue).
In the morning, the baby was reviewed by the consultant paediatrician, who noted blistering and a blackened area on the baby’s wrist. The baby was transferred to the neonatal intensive care unit at another DHB for plastic surgery review. She fortunately recovered without her injury needing plastic surgical intervention.
It was subsequently found that paediatric fluid balance charts from throughout the baby’s Bay of Plenty DHB hospital admission were not filled in regularly by staff in accordance with the DHB’s ‘Fluid balance chart recording standards (Paediatric)’ policy.
FINDINGS
- The DHB did not have a clear consensus on which IV fluid guidelines were to take priority.
- Dr D’s orientation to the IV fluid guidelines was inadequate.
- Multiple DHB staff reviewed the baby but did not recognise that the baby’s IV fluid prescription was too high.
- Multiple staff did not fill in the baby’s fluid balance chart in accordance with the DHB policy requirements.
- The HDC found that the Bay of Plenty DHB had breached the the Code of Health and Disability Services Consumers’ Rights (the Code) by failing to ensure services were provided to the baby with “reasonable care and skill”.
- It also found that RN B and RN C had both breached the Code by not providing services with “reasonable care and skill”.
- An adverse comment was made about Dr D prescribing a rate of IV fluids that was higher than the amount recommended by the guidelines.
RECOMMENDATIONS
Bay of Plenty DHB:
- Establish a clear consensus on which guidelines to be followed when prescribing IV fluids to neonates and ensure it is documented clearly.
- Provide HDC with the results of its six most recently monthly IV access audits.
- Use this case as an anonymised case study during the induction of nursing and medical staff to the Children’s Ward and Special Care Baby Unit.
- Provide a written apology to the baby’s family.
RN B:
- Undertake an audit of her compliance with fluid balance chart recording standards.
- Provide written apology to baby’s family.
RN C:
- If in future is responsible for administering IV fluids that she undertake a self-audit of the standard of her fluid balance chart documentations.
- Provide written apology to baby’s family.
The full HDC decision can be viewed here